THE INDICATIONS/NEED
Liver transplant is the treatment of choice for end-stage liver disease from cirrhosis, fulminant liver failure and non-metastatic, low tumour burden Hepatocellular Carcinoma (HCC). In Singapore, whilst Hepatitis B infection is on the decline with compulsory vaccination at birth, an emerging cause of chronic liver disease is steatohepatitis/fatty liver. Chronic liver disease in the form of cirrhosis is the catalyst for the formation of HCC (Refer to Figure 1).
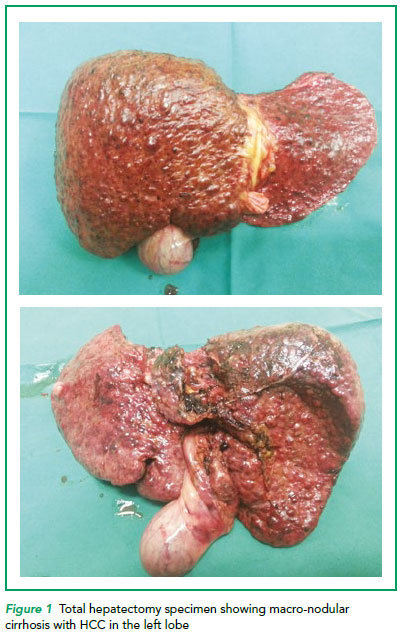
Last year, in 2017, the SingHealth Duke-NUS Liver Transplant Centre (SDDC-Liver Transplant) performed a total of 21 liver transplants, of which more than half was for HCC.
Despite the enacted HOTA for optimisation of the donor pool, actualised donor procurement is low. The small family unit with falling fertility rate does not help either in expanding the living donor pool. Till recently, most centres have used ABO compatible (ABOc) grafts, especially so in Deceased Donor Liver Transplant (DDLT), because of the risk of rejection and short preparation time.
To overcome the growing need for liver grafts and expanding indication for HCC treatment, SDDC initiated and performed Singapore’s first ABO incompatible (ABOi) Living Donor Liver Transplant (LDLT) with collaboration from various institutions.
CASE ANALYSIS
Our patient is Mr. Chen, 55-year old, with Child-Pugh B9 Hepatitis B and ethanol induced cirrhosis, complicated by HCC in the left lobe. He had prior ascites secondary to portal hypertension and spontaneous bacterial peritonitis.
A liver transplant is the treatment of choice to replace the malfunctioning liver and eradicate the hepatitis B-related tumour.
His blood group is B+ while his son who came forward as the living donor is A+. Mr. Chen’s blood plasma has anti-A antibodies which will cause reaction to the antigen A in the graft, leading to disseminated intravascular coagulation and graft death. This is the most severe form of Antibody Mediated Rejection (AMR) and will certainly result in death if there is no re-transplant. The chronic progressive form is diffuse intrahepatic biliary strictures, which also warrants re-transplant.
In order to prevent rejection of the planned right lobe graft from his son, rituximab, a specific immunosuppressive drug to deplete the B cells in Mr. Chen’s plasma as well as weaken their function in producing antibody, was administered 3 weeks prior to transplant.
It was also necessary to cleanse the blood of antibodies to the graft’s antigen A using columns of adsorption filters to very low titres. These levels were monitored daily pre and post-surgery with further apheresis when required (Refer to Figure 2).
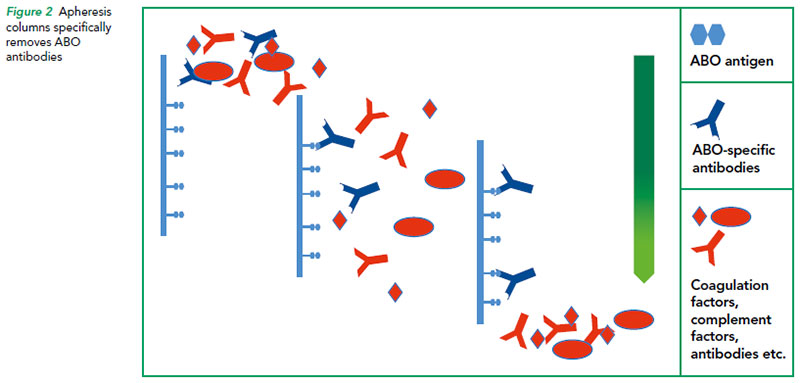
The column was coupled into haemodialysis machine to draw blood using vascular catheter inserted just prior. The apheresis took an average of 4-6 hours with minimal discomfort.
The routine immunosuppression for ABOc transplant of triple drug, i.e. steroids, mycophenolate mofetil, and tacrolimus was used. Basiliximab was used in the event tacrolimus cannot be started on time (the schematic timeline diagram depicts our ABOi protocol) (Refer to Figure 3).
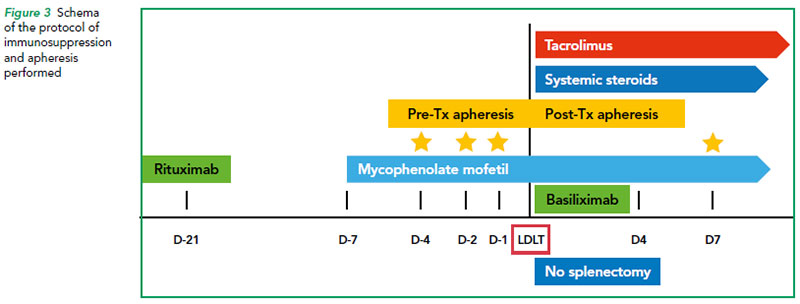
Once the liver function test returns to normal, accommodation has occurred and further apheresis is not necessary. Accommodation is the tolerance of the host towards the graft in the background of returning/normalised antibody titres, usually in a month’s time.
Mr. Chen recovered with an episode of acute cellular rejection requiring pulse steroids. He is 1 year and 3 months post-transplant and has welcomed the birth of his grandchild from his donor son and wife.
FUTURE
ABOi grafts have been routinely used as enhancement to programmes around the world to increase the donor pool. They have comparable survival results with ABOc. The desensitisation procedure has been well established and proven safe, with increasing ABOi transplant of up to 15% in high volume centres and a reported 7% complications related to the antibody related reactions.
ABOi liver transplant is possible in Singapore and can be a curative treatment for HCC. The fear of AMR can be overcome with a regimen of immunosuppression and apheresis balanced against the risk of infection.
ACKNOWLEDGEMENTS
SDDC-Liver Transplant is fortunate to work with nurses in the various wards/intensive care units and team from Department of Haematology, Renal Medicine, Renal Dialysis Centre and Blood Support Group of Health Sciences Authority of Singapore.
The SDDC-Liver Transplant team that meets every Tuesday afternoon to review clinical cases presented by primary doctors comprising of surgeon, hepatologist/physician and medical oncologist from Centre for Digestive and Liver Diseases, Singapore General Hospital and National Cancer Centre Singapore, Changi General Hospital, KK Women’s and Children’s Hospital, and Sengkang General Hospital. Liver Transplant Coordinators are available to coordinate the presentation of cases with inputs from anaesthetist, radiologist, nurses and allied health staff.
REFERENCE
1. ABOi adult LDLT under the desensitisation protocol with rituximab. Song GW, et al. Am J Transplant 2016
Professor Chung Yaw Fui Alexander is a Senior Consultant at the Department of Hepatopancreato-biliary and Transplant Surgery at the Singapore General Hospital.
He has a specialist accreditation in General Surgery and is a Senior Lecturer at the NUS
Yong Loo Lin School of Medicine.
GPs can call for appointments through the GP Appointment Hotline at
6321 4402.
Tags:
Liver
;
;
Liver;
;
Publication;News Article;
SingHealth Duke-NUS Liver Transplant Centre;
SingHealth Duke-NUS Liver Transplant Centre;
Article;
SingHealth Medical News;
;
;
SingHealth Duke-NUS Liver Transplant Centre;
;
Medical News (SingHealth)
